You’ve had a good night. Maybe it was a cold IPA at the ballpark, a glass of Cab Sav at a dinner party, or a few rounds of margaritas on a Friday. Then comes that familiar, unwelcome feeling: a burning pressure creeping up from your chest, your throat suddenly tasting sour, and the knowledge that your night isn’t quite over yet. Acid reflux has arrived.
If this sounds like you, you’re in extraordinarily common company. An estimated 40% of the U.S. population experiences GERD symptoms, with 10 to 20% of people being affected on a weekly basis. That means tens of millions of Americans, many of them social drinkers who simply enjoy a beer after work or a cocktail at a rooftop bar, are quietly suffering through heartburn that flares up like clockwork.
You Are Watching: Is Oat Milk Good For Acid Reflux Expert Advice Updated 05/2026
Somewhere along the way, oat milk entered the conversation. Maybe a friend swore by it, maybe you saw a TikTok, or maybe you just noticed it showing up in every coffee shop from Brooklyn to Bozeman. The question people are actually asking is this: can oat milk genuinely help with acid reflux, or is it just another wellness trend with a good PR team?
The answer, backed by real science, is more nuanced and more interesting than a simple yes or no. Let’s get into it.

What Is Acid Reflux and Why Does It Feel So Bad?
Before we talk about oat milk, it helps to understand what’s actually happening when acid reflux hits. At the bottom of your esophagus sits a ring of muscle called the lower esophageal sphincter (LES). Under normal circumstances, it opens to let food into your stomach and then closes tightly to keep everything from coming back up.
Acid reflux, also known as gastroesophageal reflux disease (GERD), occurs when the lower esophageal sphincter (LES) fails to close properly. This allows stomach acid to flow back up into the esophagus, leading to irritation and discomfort, including the burning sensation in the chest known as heartburn.
What starts as occasional heartburn can spiral into something far more serious. Left untreated, GERD can damage your esophagus and cause such issues as esophagitis (inflamed esophagus), Barrett’s esophagus, or even increase your risk of cancer.
GERD is a common gastrointestinal disorder with a prevalence in the U.S. ranging from 18.1% to 27.8%, with a slightly higher rate in men. That last detail is worth noting: statistically, men are somewhat more prone to erosive GERD, while women more commonly experience the non-erosive form. Either way, both sexes suffer.
The economic toll is staggering. The United States alone is estimated to spend around $10 billion annually on GERD diagnosis and treatment. This is a condition that is straining wallets and quality of life simultaneously.

The Drinking Problem Nobody Likes to Admit
Here’s where things get directly relevant for beer lovers, wine enthusiasts, and cocktail drinkers: alcohol is one of the most consistent triggers for acid reflux, and the mechanism is not subtle.
Alcohol (ethanol) directly relaxes the lower esophageal sphincter; with low LES pressure, it opens and you reflux. This isn’t a “some people are sensitive” situation; it’s basic pharmacology. The valve that’s supposed to keep your stomach acid where it belongs gets chemically loosened every time you drink.
But not all drinks are equal when it comes to reflux risk.
How Beer, Wine, and Spirits Compare
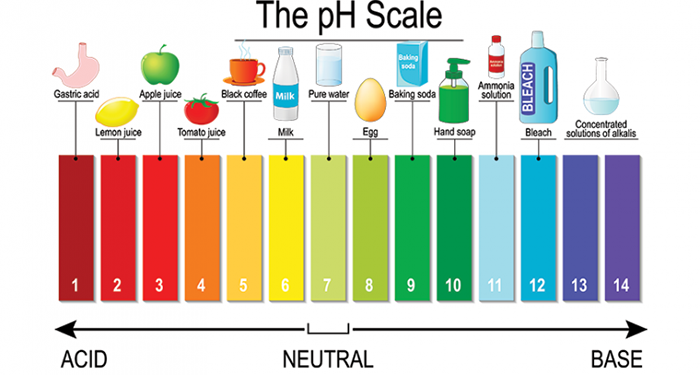
A study comparing white wine (pH 3.2) and beer (pH 4.5) found that the fraction of time at pH below 4 in the first hour after ingesting 300ml white wine was 13.2%, compared to 3.6% for beer. The study concluded that white wine and beer both induce gastroesophageal reflux, which is neither related to their ethanol content nor to their pH alone.
Beer and wine are particularly notorious for stimulating stomach acid production, thus exacerbating reflux symptoms. The carbonation in beer adds an additional insult: carbonated beverages are independently associated with GERD flares, meaning the bubbles alone can cause problems before the alcohol even enters the picture.
Research from 1993 suggests that spirits with a high ethanol content, like gin, whiskey, and cognac, may be better for people with acid reflux, as high-proof spirits are less likely to stimulate stomach acid secretion than drinks with lower ethanol content. This seems counterintuitive, but the chemistry supports it. Pure ethanol at high concentrations appears to have an inhibitory rather than stimulatory effect on gastric acid.
According to reflux specialist Dr. Jamie Koufman, when it comes to wine: red is generally better than white, and the worst whites are Chardonnay, Prosecco, and Champagne, all more acidic and with carbonation as well.
Here is a quick breakdown to help you make smarter choices at the bar:
| Drink Type | Reflux Risk | Key Reason |
|---|---|---|
| Sparkling wine / Champagne | Very High | High acidity, carbonation, low pH |
| White wine (Chardonnay) | High | Strong gastric acid stimulant |
| Beer (regular / craft IPA) | High | Carbonation, fermentation byproducts |
| Red wine | Moderate | Less acidic than whites, no carbonation |
| Cocktails with citrus | High | Citrus is a direct esophageal irritant |
| Spirits (vodka, gin, whiskey) | Lower | High ethanol inhibits acid secretion |
| Low-ABV options (Moscato) | Lower | Light-bodied, less acid stimulation |
The data makes it clear: if you enjoy a drink but deal with regular reflux, what you’re drinking matters enormously.
The Nightcap Problem
Having a nightcap, alcohol before bed, is the worst thing you can do if you have reflux. If you have a nightcap, you pretty much ensure that you will have acid reflux all night. When you lie flat, gravity is no longer on your side, and whatever the alcohol has done to relax your LES becomes far more consequential. Lying flat immediately after drinking can increase the risk that you’ll experience acid reflux at night, because alcohol can relax the lower part of the esophagus, making it easier for your stomach acid to back up.
Enter Oat Milk: The Science Behind the Hype
Oat milk has exploded in popularity across American households and coffee shops alike. The global oat milk market is now valued at nearly $3 billion, and consumption continues to climb. Part of this is environmental consciousness, part is lactose intolerance, and part is a growing awareness that it may simply be easier on the gut than dairy alternatives. For acid reflux sufferers, that last point is worth examining carefully.
Oat Milk’s Nutritional Profile
Read More : Did Pepsi Change Their Formula Updated 05/2026
Oat milk is made from a blend of oats and water. Oat milk provides a range of nutrients including vitamin D, vitamin B12, calcium, and iron. Oats themselves are low in fat, which is beneficial as high-fat foods can trigger acid reflux symptoms in some people. Additionally, oat milk is naturally free from lactose, making it a suitable option for those with lactose intolerance.
This low-fat profile is clinically significant. High-fat foods are among the best-documented acid reflux triggers because fat delays gastric emptying, meaning food (and acid) sits in your stomach longer and has more opportunities to reflux back up.
One cup of oat milk can provide up to 2 grams of fiber, which is about 8% of your daily recommended intake. That fiber content, while modest on its own, plays a meaningful role in how oat milk interacts with your digestive system.
The Beta-Glucan Advantage
The star compound in oat milk for digestive health is beta-glucan, a soluble fiber unique to oats and barley. This isn’t just marketing language; it has substantial peer-reviewed backing.
Beta-glucan plays a significant role in digestive health, mainly because it can delay gastric emptying and reduce food intake by increasing the viscosity of food in the gut. Slower gastric emptying might sound counterintuitive for reflux sufferers (since it means food sits longer), but the mechanism here is gentler and more controlled than what happens with fatty foods. The gel-like matrix that beta-glucan forms works differently, coating and buffering the digestive tract rather than overwhelming it.
Researchers found that oat beta-glucan forms a gel-like matrix in the gastrointestinal tract, increasing the viscosity of gastric and intestinal fluids. This property, combined with its resistance to enzymatic digestion, inhibits pathogenic bacterial growth. Furthermore, oat beta-glucan enhances the growth of beneficial bacteria like lactobacilli and bifidobacteria, while supporting liver health.
In plain English: the beta-glucan in oat milk doesn’t just pass through you; it actively creates a more hospitable gut environment while buffering irritants along the way.
Avenanthramides and Saponins: The Other Anti-Reflux Players
Oat milk contains avenanthramides, a unique group of antioxidants found in oats. These compounds have been shown to have anti-inflammatory properties, which can help soothe the esophagus and reduce the discomfort associated with acid reflux.
Inflammation in the esophageal lining is what causes the burning sensation to persist and intensify over time. Compounds that can reduce that inflammation at a cellular level are genuinely valuable.
The saponins present in oat milk have a protective and soothing effect on the stomach lining. These compounds can help reduce the production of stomach acid, which can alleviate acid reflux symptoms. Additionally, oat milk is easy to digest, which means that it puts less strain on the digestive system than other dairy products.
Why Dairy Milk Is Often the Wrong Choice
If you’ve ever reached for a glass of cold whole milk to soothe heartburn after a night out, you were doing what most people instinctively do. The cold liquid does feel soothing in the moment, coating the esophagus briefly and neutralizing surface acid. But the relief is temporary and can backfire.
The fat in whole milk can exacerbate stomach acid, so a low-fat version is preferable. Even though cold milk may feel good on a fiery esophagus, research supporting its use to relieve heartburn is lacking.
The fat in whole milk triggers a second wave of acid production as your stomach works overtime to process it, often making symptoms worse 30 to 45 minutes after you drank the milk in the first place. Lactose intolerance compounds the issue. When lactose ferments in the gut, it produces gas, bloating, and increased intra-abdominal pressure, all of which push stomach contents back toward the LES.
Plant-based milks like almond or oat milk are often gentler on the stomach. When choosing the best milk for acid reflux, the focus should be on low-fat options. Skim milk or plant-based alternatives like oat milk, almond milk, and soy milk tend to be better choices compared to whole milk or other full-fat options.
Oat Milk vs. Other Plant-Based Milks for Acid Reflux
Not all dairy alternatives are created equal. Here’s how oat milk stacks up against its plant-based competitors from an acid reflux standpoint:
| Milk Type | Fat Content | Fiber | pH Level | Reflux Suitability |
|---|---|---|---|---|
| Oat milk | Low | Moderate (beta-glucan) | ~6.0-7.0 | Excellent |
| Almond milk | Very Low | Low | ~8.0 (alkaline) | Very Good |
| Soy milk | Low | Low | ~7.0 | Good |
| Coconut milk (full-fat) | High | Very Low | ~6.0 | Fair (use sparingly) |
| Whole cow’s milk | High | None | ~6.5 | Poor (triggers rebound acid) |
| Oat milk (with additives) | Low | Moderate | ~6.0-7.0 | Good (check labels) |
Compared to almond milk or rice milk, oatmeal milk typically boasts a higher protein and fiber content, positioning it as a nutritionally dense option among plant-based milks. For people who want their reflux-friendly beverage to also pull nutritional weight, that matters.
However, oat milk has one caveat worth knowing about: additives. Many commercial brands add oils, thickeners like carrageenan, and sugar to improve texture and shelf life.
Carrageenan is commonly added to many nondairy beverages. It is important to note that carrageenan may cause digestive symptoms, such as bloating, irritable bowel syndrome, and inflammation. If your oat milk has a long ingredient list, you may inadvertently be adding a gut irritant back into the mix. Always check labels, and when possible, choose brands with minimal ingredients: oats, water, and perhaps a bit of salt.
Practical Ways to Use Oat Milk When Acid Reflux Strikes
Knowing oat milk is theoretically helpful is one thing; knowing how to actually use it when you’re dealing with post-drinking heartburn is another. Here are some approaches that actually work.
The Morning After
If you’ve had a few drinks the night before and wake up with a sour stomach or persistent heartburn, a glass of plain, unsweetened oat milk first thing in the morning can help. The beta-glucan creates a mild buffering effect, the low fat content means no rebound acid spike, and the warm temperature (slightly warmed, not hot) is more soothing than cold.
Beta-glucan not only supports gut health by feeding beneficial gut bacteria but also helps keep bowel movements regular. Studies indicate that beta-glucan can also reduce inflammation in the digestive tract, which can be beneficial for people with conditions like irritable bowel syndrome.
As a Mixer Alternative
If you’re managing reflux but still want to participate socially, consider using oat milk as a base for mocktails or as a creamer in your after-dinner coffee (if you choose decaf, since caffeine is also a reflux trigger). An oat milk latte with decaf espresso is significantly gentler on the esophagus than a regular dairy latte with standard espresso.
Before Bed
Read More : Does Health Ade Kombucha Have Alcohol Updated 05/2026
Low-fat or non-dairy alternatives like oat milk, almond milk, or rice milk can be gentler on the stomach than dairy milk. A small glass of oat milk before bed, particularly if you’ve had wine or cocktails earlier in the evening, can provide a mild protective coating without the fat-driven acid rebound that whole milk causes.
In Your Morning Routine
Oats and brown rice are good choices for grains as they both help you feel satisfied for longer and also help absorb stomach acid. Starting the day with oatmeal made with oat milk creates a double-dose of beta-glucan, giving your digestive system a strongly protective lining before you begin eating and drinking throughout the day.
Lifestyle Adjustments That Work Alongside Oat Milk
Oat milk is a useful tool, not a cure. For people who drink regularly and deal with chronic acid reflux, a few additional adjustments can substantially reduce how often reflux strikes.
Timing is everything. Avoiding drinking alcohol 2 to 3 hours before bed can significantly reduce the risk of nighttime acid reflux, since lying flat after drinking allows stomach acid to more easily back up into the esophagus.
Watch the mixers. Cocktails made with citrus juice, tomato juice, or carbonated sodas combine multiple reflux triggers simultaneously. A vodka soda is considerably less problematic than a Bloody Mary or a Margarita with fresh lime.
Eat before you drink. An empty stomach intensifies alcohol’s effect on the LES. A small meal with complex carbohydrates and lean protein before drinking can meaningfully buffer the impact. Foods like oatmeal, bananas, and whole grain bread are particularly good pre-drink choices for reflux sufferers.
Track your personal triggers. Keeping a journal of all the foods and drinks you consume can help you spot a pattern between drinking a certain beverage and your symptoms, allowing you to cut back on specific items to minimize GERD symptoms. Acid reflux is surprisingly individual. Some people can tolerate red wine but not white; others find beer worse than spirits. Data from your own body is the most valuable data you have.
Watch your portion sizes. Limiting alcohol intake to no more than the equivalent of a 12-ounce regular beer, 8 to 9 ounces of malt liquor, a 5-ounce glass of wine, or one 1.5-ounce pour of distilled liquor can help manage GERD symptoms while still enjoying alcoholic beverages.
When to Take It Seriously: The Line Between Heartburn and GERD
Not all reflux is the same, and knowing where your symptoms fall on the spectrum matters.
Occasional heartburn from acid reflux isn’t likely a cause for concern, but you should contact a gastroenterologist if your symptoms occur more than twice a week and become more than just an annoyance. That’s the clinical threshold: twice a week is where occasional discomfort becomes a condition requiring medical attention.
While lifestyle changes and medications from the proton pump inhibitor (PPI) family are commonly used to treat GERD, medically resistant GERD has become an increasing challenge. This means that for a growing number of people, over-the-counter antacids and even prescription PPIs aren’t delivering complete relief. Dietary interventions, including switching to oat milk, are increasingly being explored as complementary approaches precisely because medications alone often aren’t enough.
If you smoke, are overweight, or take medications like antihistamines or antidepressants regularly, your reflux risk is compounded. People who drink and use tobacco or nicotine products have a greatly increased risk of developing respiratory and digestive tract diseases, including cancer of the mouth, throat, lung, or esophagus. The adverse interaction between tobacco and ethanol is synergistic.
Choosing the Right Oat Milk: What the Label Should (and Shouldn’t) Say
Not all oat milks are made equal, and if you’re using it specifically to manage acid reflux, quality and ingredient transparency matter.
Look for: Short ingredient lists (ideally oats, water, and minimal additions), no carrageenan, low added sugar, and no artificial flavors or preservatives.
Be cautious of: “Barista edition” formulas with added oils for frothing, sweetened varieties (added sugar can independently worsen reflux), and products with carrageenan listed in the ingredients.
Brands commonly noted for clean formulations include Oatly (original, not the barista version), Minor Figures, and Elmhurst 1925 Oat Milk, though you should always verify current formulations, as brands update their recipes.
Making oatmeal milk at home allows you to manage the ingredients, potentially avoiding any additives present in certain store-bought varieties. It might be beneficial for acid reflux management by ensuring a clean, uncomplicated option. Homemade oat milk is simple: soak rolled oats in water for 30 minutes, blend, and strain. You control exactly what goes in.
The Bottom Line from a Gut Health Perspective
Oat milk is genuinely one of the better beverage choices for people managing acid reflux, particularly those who also drink alcohol socially. It works through several complementary mechanisms: the low fat content avoids rebound acid production, the beta-glucan creates a soothing gel-like buffer in the digestive tract, avenanthramides reduce esophageal inflammation, and saponins help regulate stomach acid production. It is also lactose-free, removing one of the most common indirect triggers of acid-related discomfort.
That said, oat milk isn’t a free pass to ignore everything else. While oat milk may be a helpful natural remedy for acid reflux, it is not a substitute for medical treatment. If you experience any adverse effects, such as increased acid reflux symptoms, discontinue use and speak with your healthcare provider.
For anyone who enjoys beer, wine, or cocktails but battles the burning aftermath, oat milk represents something practical and evidence-adjacent: a low-risk, widely available, genuinely useful addition to your toolkit for managing how your gut responds to the things you enjoy.
A Note on the Bigger Picture
Here is something worth sitting with: the real conversation isn’t “oat milk vs. antacids” or “oat milk vs. alcohol.” It’s about building habits that let you participate in a life you actually enjoy without your digestive system staging a protest.
For the person who loves a cold craft beer at a Friday night cookout, a glass of Barolo at a nice Italian dinner, or a well-made Old Fashioned at a bar with a great bartender, the goal isn’t abstinence. It’s strategy. Choose lower-risk drinks when you can, eat before you drink, don’t lie down immediately after, and incorporate genuinely helpful foods and beverages (oat milk among them) into your daily routine.
The burning in your chest is a signal from your body, not a judgment. Listening to it, and responding intelligently, is what makes the difference between suffering through the night and sleeping soundly.
Sources: https://chesbrewco.com
Category: Drink